| ⚕️ Supplement Disclosure This article reviews magnesium as a dietary supplement for informational purposes only. Adults with diagnosed atrial fibrillation, other arrhythmias, kidney disease, or those taking blood pressure medications, diuretics, or digoxin should consult their physician before starting any magnesium supplement. Magnesium can affect the absorption and action of several medications. This article does not constitute medical advice and is not a substitute for care from a qualified cardiologist or physician. |
Your heart beats approximately 100,000 times per day. Every single contraction depends on magnesium. The mineral acts as a natural calcium channel regulator — controlling how much calcium enters cardiac cells to trigger contraction — and plays a direct role in maintaining vascular tone, electrical conduction, and blood pressure regulation.
Despite this, an estimated 45–50% of Americans are deficient in magnesium, with rates higher in adults over 50 due to reduced dietary intake, decreased gut absorption with age, and medication-induced losses from diuretics and proton pump inhibitors. The cardiovascular consequences of this silent deficiency are well-documented: higher rates of hypertension, arrhythmia, and cardiovascular mortality in people with low serum magnesium.
This guide covers the three magnesium forms most relevant for heart health and blood pressure, what the 2025 research actually shows, which form to choose based on your specific concerns, and five products available at US retailers with 2026 pricing.
| The Clinical Story in Brief A 2025 meta-analysis in Hypertension (38 RCTs, 2,709 participants) found magnesium supplementation reduced systolic blood pressure by −2.81 mmHg and diastolic by −2.05 mmHg overall. In hypertensive individuals and those with confirmed magnesium deficiency, reductions were substantially larger: −7.68 mmHg systolic in hypertensive patients on BP medications. A 2024 umbrella meta-analysis (8,610 participants across 10 review papers) confirmed consistent SBP and DBP reductions, with the greatest effect at doses ≥400mg/day. |
Why Magnesium Matters Specifically for Cardiovascular Health
Magnesium operates at the intersection of three cardiovascular mechanisms that are most compromised in adults over 50:
1. Blood Pressure Regulation
Magnesium relaxes vascular smooth muscle by competing with calcium at channel entry points — the same mechanism exploited by calcium channel blocker medications like amlodipine. When magnesium levels are low, vascular tone increases and blood pressure rises. The 2025 Hypertension meta-analysis confirmed this dose-response relationship across 38 trials, with the most pronounced effects in adults who were both hypertensive and magnesium-deficient.
2. Cardiac Rhythm and Arrhythmia Prevention
Magnesium is essential for the stability of electrical conduction in the heart. The Framingham Heart Study found that low serum magnesium was independently associated with a significantly increased risk of atrial fibrillation (AFib) in community-dwelling adults. A 2023 meta-analysis in PLoS One (PloS ONE, Curran et al.) confirmed that magnesium prophylaxis reduced the incidence of new-onset AFib in surgical patients. A 2018 analysis of 22 studies found magnesium reduced the risk of both ventricular and supraventricular arrhythmias.
Up to 38% of adults with ventricular arrhythmias have confirmed magnesium deficiency. The connection is mechanistic: without adequate magnesium, potassium and sodium channel function is disrupted, creating the electrical instability that underlies ectopic beats and arrhythmias.
3. Endothelial Function and Arterial Stiffness
Low magnesium is associated with increased oxidative stress in vascular endothelial cells, elevated C-reactive protein (CRP), and greater arterial stiffness — three independent markers of cardiovascular disease risk. Multiple studies confirm that magnesium supplementation reduces inflammatory markers and improves endothelial function in adults over 50.
Which Magnesium Form Is Best for Heart Health?
| Form | Heart Health Use | Absorption | Best For | GI Tolerance |
| Magnesium Taurate | ★★★ — cardiovascular-specific (taurine synergy) | Good | Blood pressure, arrhythmia, palpitations | Excellent |
| Magnesium Glycinate | ★★ — broad cardiovascular support | Excellent | BP, sleep, general deficiency | Best in class |
| Magnesium Malate | ★★ — energy + BP | Good | Fatigue + cardiovascular combo | Very Good |
| Magnesium Citrate | ★ — primarily bowel/general | Good | Constipation, general repletion | Moderate (loose stool at high dose) |
| Magnesium Oxide | ✗ — avoid for heart health | Poor (~4%) | Antacid use only | Poor |
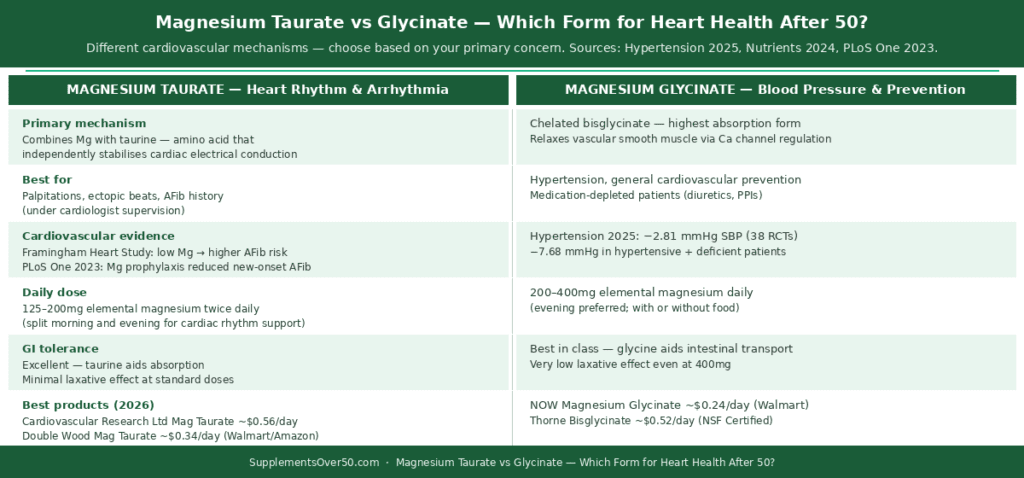
Magnesium Taurate — The Heart-Specific Form
Magnesium taurate combines magnesium with taurine — an amino acid with its own independent cardiovascular benefits. Taurine regulates calcium signalling in cardiac muscle, supports GABA activity (reducing sympathetic nervous system tone on the heart), and has demonstrated blood pressure-lowering and anti-arrhythmic effects in multiple human studies. The combination produces synergistic cardiovascular support beyond magnesium alone.
Cardiovascular Research Ltd’s magnesium taurate has been used by cardiologists for arrhythmia support for over two decades, and it is frequently cited in AFib patient communities as one of the more consistently effective approaches for reducing palpitations and ectopic beats. The dose most studied for AFib support is 125–200mg elemental magnesium (as taurate) twice daily.
| ⚠️ AFib and Arrhythmia — Medical Supervision Required If you have been diagnosed with atrial fibrillation or any other arrhythmia, any change in supplementation — including magnesium — should be discussed with your cardiologist before starting. Many AFib patients are on anticoagulants or antiarrhythmic medications that interact with supplements. Magnesium is generally well-tolerated alongside most cardiovascular medications, but your specific medication list requires individual review. |
Magnesium Glycinate — Best All-Round Absorption and Tolerance
For adults who want the best-absorbed magnesium for general cardiovascular support without the specific arrhythmia focus, glycinate remains the gold standard. It is chelated to glycine, which escorts magnesium through intestinal cell membranes via a different pathway than ionic magnesium — dramatically reducing laxative effects and producing more consistent blood magnesium elevation at lower doses. Elemental magnesium content is ~14% by weight.
Who Should Choose Which Form
| Your Primary Concern | Recommended Form |
| Palpitations, ectopic beats, AFib history | Magnesium Taurate (125–200mg elemental, twice daily) — discuss with cardiologist |
| High blood pressure (hypertension) | Magnesium Glycinate or Taurate — both effective; glycinate better tolerated at higher doses |
| General cardiovascular prevention over 50 | Magnesium Glycinate 200–400mg daily — best value and tolerability |
| Fatigue alongside BP concerns | Magnesium Malate — malic acid supports mitochondrial energy (Krebs cycle) |
| On diuretics / depleted by medication | Magnesium Glycinate at 400mg daily — highest priority in this group |
What the 2025 Research Shows — Key Studies
- Hypertension 2025 (38 RCTs, n=2,709): Magnesium supplementation reduced systolic BP by −2.81 mmHg and diastolic by −2.05 mmHg. In hypertensive patients on BP medications, systolic reduction was −7.68 mmHg. In hypomagnesaemic individuals, systolic reduction was −5.97 mmHg. No dose-response relationship was found, suggesting that correcting deficiency matters more than the exact dose.
- Nutrients 2024 (subgroup meta-analysis): Magnesium at ≤360mg/day for >3 months reduced systolic BP by −4.31 mmHg. Duration of supplementation (>3 months) produced larger effects than higher doses over shorter periods.
- PLoS One 2023 (Curran et al.): Magnesium prophylaxis significantly reduced new-onset AFib incidence. The authors concluded magnesium has a role in arrhythmia prevention, particularly in deficient populations.
- Framingham Heart Study: Low serum magnesium (<0.77 mmol/L) was independently associated with a significantly higher risk of developing AFib over a 20-year follow-up in community adults — a landmark dataset establishing deficiency as a modifiable risk factor.
- Current Therapeutic Research 2024 (umbrella meta-analysis, 8,610 participants): Confirmed significant reductions in both SBP and DBP from magnesium supplementation, with greater effects in subjects receiving ≥400mg/day.
5 Best Magnesium Supplements for Heart Health — US Pricing 2026
1. Cardiovascular Research Ltd Magnesium Taurate — Amazon — Best for Arrhythmia Support
Best for: seniors with palpitations, ectopic beats, or AFib history (under cardiologist guidance).
| Formula | 125mg elemental magnesium per capsule (as magnesium taurate) |
| Price (2026) | ~$22–28 for 90 capsules (~$0.49–0.62/day at 2 caps) |
| Third-Party Tested | GMP certified; the original clinical-grade magnesium taurate formula; used by cardiologists for 20+ years |
| Best For | AFib patients and those with palpitations — discuss dose and timing with your cardiologist |
| Notes | Lower elemental magnesium percentage (taurate form) — take twice daily for full cardiovascular effect |
2. Double Wood Supplements Magnesium Taurate — Amazon / Walmart — Best Value Taurate
Best for: seniors wanting magnesium taurate at a lower price point than the Cardiovascular Research brand.
| Formula | 125mg elemental magnesium per 2 capsules (as magnesium taurate) |
| Price (2026) | ~$18–22 for 120 capsules (~$0.30–0.37/day at 2 caps) |
| Third-Party Tested | Third-party tested for purity; Non-GMO; manufactured in FDA-registered facility |
| Best For | Budget-conscious seniors seeking magnesium taurate specifically for cardiovascular support |
| Notes | Good option if cost is a barrier to the Cardiovascular Research brand; widely available on Amazon |
3. NOW Foods Magnesium Glycinate — Walmart / Amazon — Best Overall Value
Best for: general blood pressure support and cardiovascular prevention at the lowest cost per dose.
| Formula | 200mg elemental magnesium per 2 capsules (as bisglycinate chelate) |
| Price (2026) | ~$20–24 for 180 capsules at Walmart (~$0.22–0.27/day) |
| Third-Party Tested | NOW IGEN Non-GMO; GMP certified facility; NSF registered |
| Best For | Blood pressure support, general magnesium deficiency repletion, excellent GI tolerance |
| Notes | Best cost-per-serving in this category; can be taken at 400mg/day (2 servings) for stronger BP effect |
4. Thorne Magnesium Bisglycinate — Thorne.com / Amazon — Best NSF-Certified
Best for: seniors who want the highest-certification magnesium glycinate — physician-grade quality.
| Formula | 200mg elemental magnesium per 2 capsules (bisglycinate chelate) |
| Price (2026) | ~$28–34 for 60 servings (~$0.47–0.57/day) |
| Third-Party Tested | NSF Certified for Sport — highest available certification |
| Best For | Seniors on multiple medications who want the most rigorously tested magnesium available |
| Notes | Same form as NOW at a premium; the NSF certification provides pharmaceutical-grade quality assurance |
5. Life Extension Magnesium Caps — LifeExtension.com / Amazon — Best Triple-Form Blend
Best for: seniors who want broad magnesium coverage from multiple forms in one capsule.
| Formula | 500mg magnesium oxide + citrate + succinate blend per 2 capsules (~160mg elemental Mg) |
| Price (2026) | ~$12–16 for 100 servings (~$0.12–0.16/day) — excellent value |
| Third-Party Tested | Non-GMO; manufactured in Life Extension’s NSF-registered facility |
| Best For | Budget-conscious seniors wanting multiple forms; note oxide component reduces overall absorption |
| Notes | The citrate and succinate fractions are well-absorbed; oxide less so — an acceptable compromise at this price point |
Dosing Guide — Magnesium for Heart Health After 50
| Concern | Form | Daily Dose | Notes |
| General BP prevention | Glycinate | 200–400mg | Evening dose preferred; with or without food |
| Active hypertension | Glycinate or taurate | 300–400mg | Discuss with physician; may complement BP meds |
| Palpitations / ectopic beats | Taurate | 125–200mg twice daily | Split morning and evening; discuss with cardiologist |
| On diuretics (depleted) | Glycinate | 400mg | Space 2hrs from diuretic dose; test serum Mg |
| General cardiovascular prevention | Glycinate or malate | 200–300mg | Consistent daily use; 3+ months for full BP effect |
Important: space magnesium at least 2 hours from antibiotics (fluoroquinolones, tetracyclines), bisphosphonates (alendronate/Fosamax), and thyroid medication (levothyroxine), as magnesium reduces absorption of all of these.
Related Articles on SupplementsOver50.com
• Magnesium Glycinate vs Citrate — Which Form Is Better for Seniors After 50?
• Best Magnesium Supplement for Sleep After 50: Glycinate vs L-Threonate
• Best Magnesium Supplement for Leg Cramps at Night After 50
• Heart Health Supplement Stack for Seniors — CoQ10, Omega-3 and Magnesium
• Ubiquinol vs CoQ10 — Is the More Expensive Form Worth It After 60?
• The 5 Essentials — Supplements Every Adult Over 60 Should Know
References
1. Hypertension 2025: Magnesium supplementation and blood pressure meta-analysis (38 RCTs, n=2,709)
2. Nutrients 2024: Magnesium and potassium for systolic BP reduction — subgroup meta-analysis
5. Framingham Heart Study: Low serum magnesium and risk of atrial fibrillation in community adults
6. Antioxidants 2020: Magnesium, oxidative stress, inflammation, and cardiovascular disease — review
Frequently Asked Questions
How much does magnesium actually lower blood pressure?
According to a 2025 meta-analysis of 38 clinical trials, magnesium supplementation reduces systolic blood pressure by an average of 2.81 mmHg and diastolic by 2.0 mmHg across all participants. The effect is significantly larger in those who are hypertensive or magnesium-deficient — reductions of up to 7.68 mmHg systolic have been documented in deficient adults, which is clinically meaningful for reducing stroke and cardiovascular event risk. For context, a 5 mmHg reduction in systolic blood pressure is associated with a 14% lower risk of stroke death and 9% lower risk of coronary heart disease death in population studies.
Is Magnesium Taurate safe to take with AFib?
Adults with diagnosed atrial fibrillation must consult their cardiologist before starting any magnesium supplement. Magnesium influences cardiac electrical conduction and can interact with antiarrhythmic medications (flecainide, amiodarone) and anticoagulants (warfarin, Eliquis). If cleared by a physician, Magnesium Taurate is often the preferred form for cardiac rhythm concerns — taurine has independent antiarrhythmic properties including stabilising cardiac membrane potential and reducing oxidative stress on the myocardium. Start at 200mg daily and increase only under physician supervision.
How long does it take for magnesium to help the heart?
Timeline varies by outcome. Subjective improvements — reduced palpitations, better sleep, fewer muscle cramps — often appear within 2–4 weeks as tissue magnesium stores begin to replenish. Measurable blood pressure reductions typically require 8–12 weeks of consistent daily use for full effect on vascular tone. The 2025 meta-analysis showing the 2.81 mmHg reduction used trials averaging 12 weeks duration. Consistency matters more than dose — magnesium taken daily for 3 months produces greater cardiovascular benefit than sporadic high-dose use.
Does magnesium lower blood pressure in seniors?
Yes — the 2025 Hypertension meta-analysis of 38 randomized controlled trials found magnesium supplementation reduced systolic blood pressure by 2.81 mmHg and diastolic by 2.05 mmHg on average. The effect was substantially larger in hypertensive individuals (−7.68 mmHg systolic) and those with confirmed magnesium deficiency (−5.97 mmHg systolic). While 2–3 mmHg may not sound large, sustained reductions of this magnitude are associated with an 8% lower risk of stroke and 5% lower cardiovascular mortality in population studies. Magnesium is not a replacement for antihypertensive medication in people with diagnosed hypertension, but it is a meaningful complement under physician guidance.
Is magnesium taurate better than glycinate for heart health?
For specifically cardiovascular applications — particularly palpitations, ectopic beats, and atrial fibrillation risk — magnesium taurate has the edge due to the added cardiovascular benefits of taurine, which independently supports cardiac rhythm and blood pressure. For general blood pressure support and broad cardiovascular prevention without specific arrhythmia concerns, magnesium glycinate is equally effective and significantly better tolerated at higher doses. Adults with AFib should discuss both options with their cardiologist, as the choice may depend on their medication list.
Can magnesium help with atrial fibrillation?
Magnesium plays a documented role in cardiac electrical stability, and low magnesium is independently associated with higher AFib risk based on the Framingham Heart Study data. A 2023 meta-analysis found magnesium prophylaxis reduced new-onset AFib in certain populations. However, magnesium supplementation is not an approved treatment for AFib and cannot replace antiarrhythmic medications or anticoagulation therapy prescribed by a cardiologist. If you have diagnosed AFib, discuss magnesium supplementation with your cardiologist — it may be a useful adjunct but requires individual assessment.
How long does it take for magnesium to lower blood pressure?
The 2024 Nutrients meta-analysis found that magnesium supplementation for more than 3 months produced larger blood pressure reductions than shorter courses, with a mean systolic reduction of −4.31 mmHg at >3 months. Most individuals notice subjective changes — reduced muscle tension, better sleep quality, fewer palpitations — within 4–8 weeks. Blood pressure monitoring after 8–12 weeks of consistent use is the appropriate way to evaluate cardiovascular effectiveness.
Does magnesium interact with blood pressure medications?
Magnesium at standard supplemental doses (200–400mg elemental/day) is generally safe alongside most antihypertensive medications, including ACE inhibitors, ARBs, beta-blockers, and calcium channel blockers. In some cases, magnesium may complement the blood pressure-lowering effect of these medications — which means monitoring is sensible when starting supplementation in someone already on treatment. The most important interaction caution is with diuretics: thiazide and loop diuretics deplete magnesium, making supplementation more important in this group, but their effect on electrolyte balance warrants physician oversight.
The Bottom Line
Magnesium is the most clinically supported non-prescription intervention for blood pressure support in adults over 50 — and the only supplement with 38 RCTs specifically examining its blood pressure effects in the most recent meta-analysis. The cardiovascular case goes beyond blood pressure: its role in cardiac electrical stability, arrhythmia prevention, and endothelial function makes it foundational for any supplement approach to heart health after 50.
For general cardiovascular prevention, NOW Magnesium Glycinate at Walmart (~$0.24/day) is the highest-value entry point. For seniors specifically concerned about palpitations, ectopic beats, or with AFib history under cardiologist supervision, Cardiovascular Research Ltd Magnesium Taurate (125mg twice daily) is the form with the longest clinical track record for arrhythmia support.


